What is Age-related Macular Degeneration?
Age-related Macular Degeneration (called ‘AMD’ on this website) is an eye diseases that affects the macula, the part of the retina needed for sharp, central vision. AMD causes gradual blurring or loss of central vision but does not affect side (peripheral) vision or cause total black blindness. Losing central vision can make it harder to see faces, read and drive. Early signs of AMD may be present without you noticing.
Around 1.4 million Australians aged 50 and over have AMD1 – that’s around 1 in 7 people. 20% of patients with early AMD will progress to advanced (late stage disease) within 5 years2.
Once vision is lost to AMD, it cannot be restored. However, there are steps you can take to keep your macula healthy and slow down the disease if it’s detected early.
AMD has a strong genetic component. Family members of people with AMD have a higher risk of the condition3.

SightScore AMD is an age-related macular degeneration genetic risk service. This service is currently only available in Australia and New Zealand.
What are the main risk factors for AMD?
The risk that a person will develop AMD in the future, or that already-diagnosed AMD will get worse, depends on a wide range of factors. These include:
- Risk factors such as an age over 50, a family history of AMD, or European ancestry.
- Clinical features such as large drusen, pigmentary abnormalities, and drusen volume.
- Variations in genes that influence your risk of AMD.
- Not having regular eye exams. If you’re at risk of AMD, it’s important to have regular eye exams including a check of your macula. Early AMD doesn’t have symptoms, so don’t wait for your vision to change.
How can genetics be used to assess AMD risk?
Humans share the same genetic code apart from some differences, called genetic variants, that make each of us unique. Some of these variants are known to increase the risk of developing health conditions like AMD, while others reduce the risk. It is possible to combine the risks from these genetic variants to estimate a person’s genetic risk of developing AMD in future or, if they already have AMD, the risk their AMD might get worse, relative to others in the community.
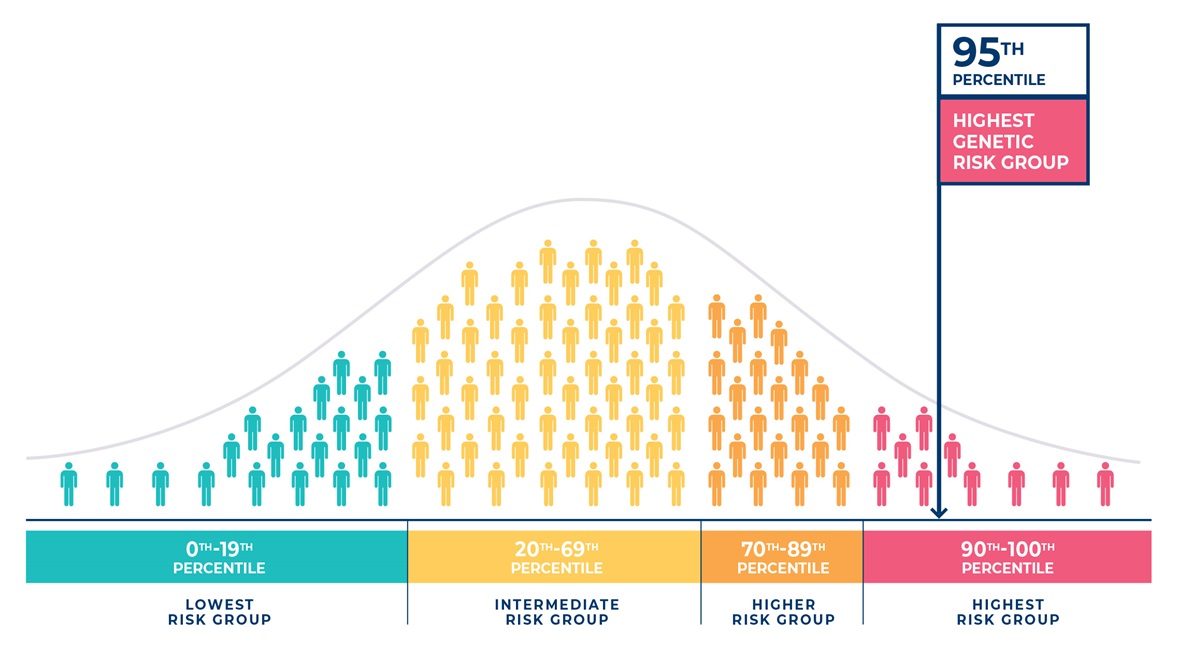
How does genetic risk relate to family history?
Blood relatives (e.g. parents, brothers/sisters, children) share parts of their genetic code and will have some of the same genetic variants. Thus, for diseases with a strong genetic contribution, such as AMD, an eye health professional will take account of a person’s family history when assessing their risk.
However, a family history is not the same as a person’s individual genetic risk. It is possible to have a high genetic risk of AMD without a family history of the disease. It is also possible to have a family history of AMD and have a low individual genetic risk.
This is because a family history does not mean a person has personally inherited the genetic variants that increase the risk of AMD.
Analysing a person’s unique genetic code may provide a health practitioner additional information about an individual’s risk of developing AMD relative to others with a family history of AMD.
How is genetic testing performed?
Genetic testing may be performed by collecting a saliva sample, extracting the DNA inside, and then analysing genetic results.
SightScoreTM is a clinical genetic testing service provided by Seonix Bio, based on an accredited genetic risk score. It estimates a person’s genetic risk of developing AMD in future or, if they already have AMD, the risk their AMD might get worse, relative to others in the community.
How can AMD risk information be used by a healthcare practitioner?
Depending on your medical history and eye examination, your healthcare practitioner may use SightScore-AMD to consider:
- When you should first be checked for AMD.
- How often you should be checked for AMD.
- How to manage your care if you have AMD, including lifestyle modifications and some treatment decisions.
- Whether your close blood relatives (e.g. parents, siblings, adult children) should be checked for AMD.
SightScore-AMD may also be used to help you understand your personal genetic risk. This will allow you to be proactive in your healthcare in regard to any recommendations about follow-up appointments and lifestyle changes that might be worthwhile.
What can be done about AMD risk?
The most important thing is to follow the advice of a healthcare practitioner and particularly, to attend regular eye health check-ups. To keep your macula healthy, recommendations include not smoking, regular exercise, maintaining healthy blood pressure and cholesterol levels and an eye-healthy diet4.
References
- Keel S, Xie J, Foreman J, et al. Prevalence of age-related macular degeneration in Australia. The Australian National Eye Health Survey. JAMA Ophthalmol. 2017; 135(11):1242-9.
- Gehrs KM, Anderson DH, Johnson LV, Hageman GS. Age-related macular degeneration–emerging pathogenetic and therapeutic concepts. Ann Med. 2006;38(7):450-71.
- Klaver CCW, Wolfs RCW, Assink JJM, et al. Genetic Risk of Age-related Maculopathy Population-Based Familial Aggregation Study. JAMA Ophthalmol. 1998; 116(12):1646-51.
- Optometry Australia. Clinical Practice Guide for the Diagnosis and Management of Age-related Macular Degeneration. 2024. https://www.optometry.org.au/wp-content/uploads/Professional_support/Guidelines/2024-AMD-Clinical-Practice-Guide-v11-Compressed-Copy.pdf
Frequently asked questions
Humans share the same genetic code apart from some differences, called genetic variants, that make each of us unique. Some of these variants are known to increase the risk of developing certain health conditions, while others reduce the risk. It is possible to combine the risks from thousands or millions of these genetic variants to estimate the overall risk of a person developing a particular health condition, such as glaucoma or age-related macular degeneration. This overall risk is known as a polygenic risk score. In some cases, a polygenic risk score may also be linked to the potential severity of the health condition and the way it might develop over time.
SightScore is a saliva test that looks at many genetic variants in your DNA to estimate your genetic risk of developing an eye disease in the future, or if you already have the eye disease, the risk that your disease might get worse, relative to others in the community with similar ancestry. It has received regulatory approval by the National Association of Testing Authorities (NATA) for use in Australia and New Zealand.
Blood relatives – e.g. parents, brothers/sisters, adult children – share parts of their genetic code and will have some of the same genetic variants, and some that are different. For conditions with a strong genetic contribution, such as glaucoma or AMD, a healthcare practitioner will take into account a person’s family history when assessing their risk.
However, a family history is not the same as a person’s individual genetic risk. It is possible to have a high genetic risk of eye disease without a family history of the condition. It is also possible to have a family history of an eye disease and have a low individual genetic risk. This is because a family history does not mean a person has personally inherited the genetic variants that increase the risk of disease.
SightScore is a personalised test which uses a person’s own DNA to assess their individual genetic risk of developing eye disease. Analysing a person’s unique genetic code may provide a health practitioner additional information about an individual’s risk of developing disease relative to others with a family history.
SightScore does not account for: age, family history or environmental factors.
SightScore only estimates genetic risk. It does not take these other things into account. However, a healthcare practitioner will consider them when advising about future health care.
In most people, the risk of developing a particular eye disease is influenced by many common genetic variants. Most of these variants contribute a small amount individually to the risk of developing each eye disease, though some may contribute more significantly. The SightScore test looks at many of these variants, to estimate overall risk. Occasionally, a person will have a very rare single variant in a key gene that has a large impact on the risk of developing a particular disease. SightScore does not test for these rare variants.
In certain cases – for example, if there is a strong family history or other clinical features – your healthcare provider may recommend separate testing for these rare variants.
Seonix complies with the most stringent local and international privacy and security regulations. We take incredible care to use technical, process and physical safeguards to secure your personal information and protect it against misuse, loss or alteration.
We only disclose your personal information where it is necessary to provide our products and services to you or for other legitimate purposes described in our Privacy Policy.
You can be referred for a SightScore AMD test by your optometrist or ophthalmologist.
Seonix or your health practitioner will give you a SightScore test kit. This kit contains a saliva swab collection tube and instructions on how to collect your saliva sample. Follow the instructions to collect and submit your sample.
If you would like additional help, please watch the video below:
https://www.dnagenotek.com/row/support/collection-instructions/oracollect-dna/OCR-100.html
Please go to www.seonixbio.com/register and follow the SightScore Registration and Collection Instructions provided with your kit. You will need your Referral ID number which has been sent to you via SMS and email.
Please check that you are entering the correct Referral ID, name and date of birth. These must exactly match the details in the referral from your health practitioner. You can check which first and last name were used on the referral by looking at the email and SMS correspondence we send you. If you are having problems it is worth checking if the first and last name on your referral have been mixed up, a spelling error has been made, or if you use more than one first name (e.g. an English version and a non-English version) please make sure you use the version of your name used on the referral. Please contact support@seonixbio.com if you continue to have problems.
Some people will pay for their test at their health practitioners, whilst others will pay for their test online. For those patients who are paying Seonix online for their test they will be sent a payment link via email. If you do not receive this link you can go to www.seonixbio.com/pay and enter your Referral ID, which you will have received via SMS and email.
Once our laboratory receives your saliva sample, they isolate your DNA and analyse up to millions of locations across your genome to find genetic variants that either increase or decrease your risk of developing eye disease. SightScore combines the effects of these variants and compares your score to others in the community with similar ancestry.
Once your sample has arrived at our laboratory, it typically takes 4-6 weeks for your results to become available. If you were referred by a health practitioner, your results will be returned to them and they will share them with you. If you ordered your test through our SightScore Family service, then you will receive an email when your results are ready to be downloaded.
SightScore is not covered by Medicare or private health insurance at this time. You will need to pay for your kit either at your health practitioner or at the time of kit registration. We will not process your sample if you have not paid for your test.
Genetic testing can have an impact on some types of insurance, particularly life insurance. There is currently a moratorium on genetic tests in life insurance, which means that genetic test results cannot be used as part of an insurance application up to the value of $500,000 (for death and total permanent disability), $200,000 for trauma and $4,000 a month for income protection.
For more information, please see Centre for Genetics Education or Financial Services Council websites.